
Bacteria are increasingly developing resistance to antibiotics, a phenomenom that began decades ago and is already having a major impact. In 2023, antibiotic resistance was linked to 24.000 deaths in Spain and more than 4.5 million worldwide. Recent international and national data point to an even more worrying future. If current trends continue, by 2050 Spain could see around 45.000 deaths per year related to antibiotic resistance, close to 10% of all deaths and roughly one third of those attributed to cancer. These figures highlight an alarming reality: antiniotics are losing their effectiveness, and as a result, infections that were once easy to treat may become serious health threats that are increasingly difficult to control.
Spain is one of the highest consumers of antibiotics in Europe [Fig. 1]. Use began to decline before the pandemic, and although it rose again in the years that followed, the level recorded in 2023 was lower than in 2016, placing Spain among the countries that have achieved the largest reductions. Behind this still-high level of consumption are practices such as self-medication, unnecessary prescriptions, stopping treatments too early, and the widespread use of antibiotics in livestock farming. Together, these patterns point to insufficient public awareness and understanding, which in turn accelerates the loss of effectiveness of medicines that are essential for public health.
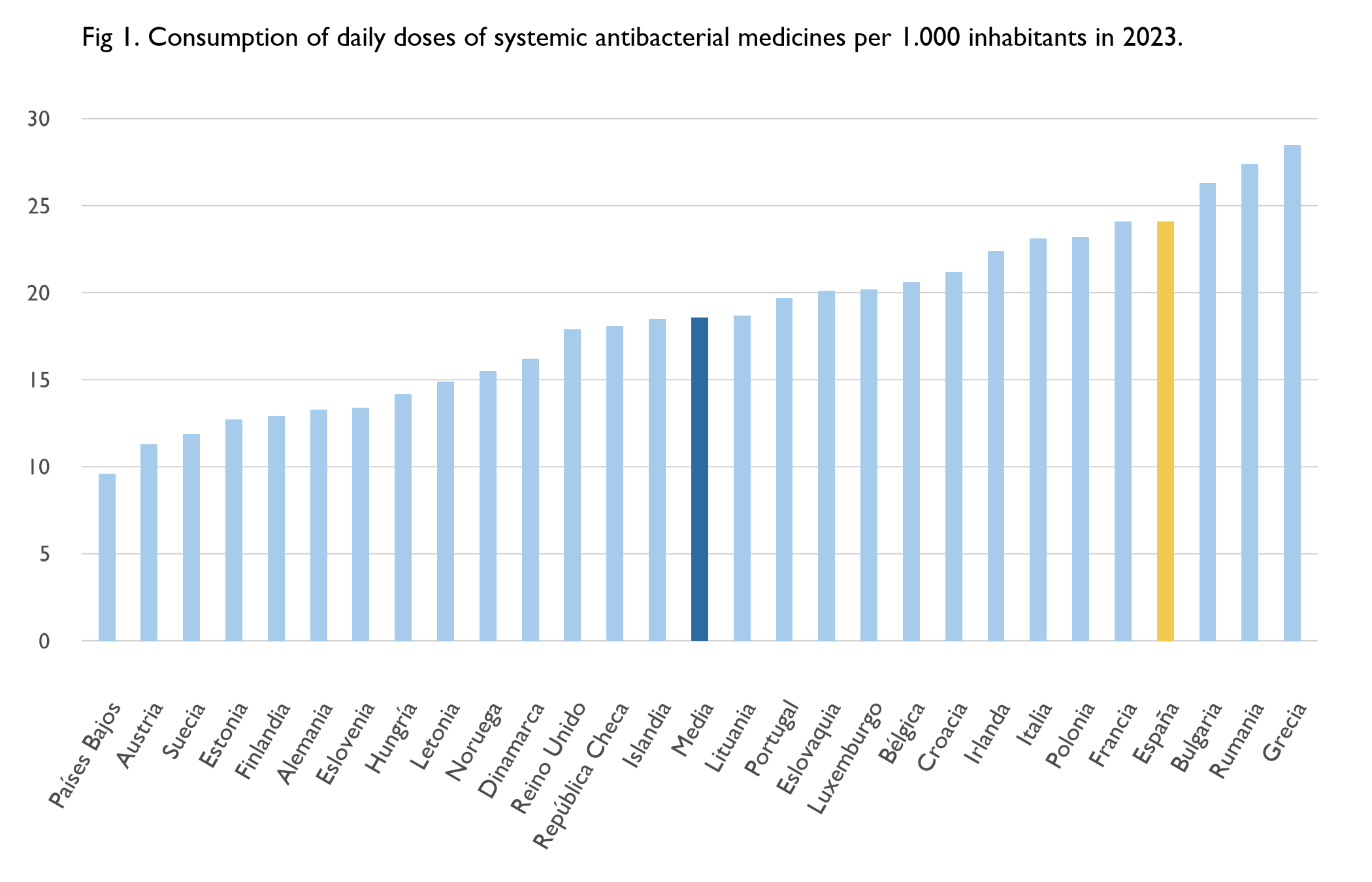
Source: own analysis based on OECD data.
The good news is that there is still time to reverse this trend. Ensuring proper access to antibiotics and promoting their responsible use are essential to preserving their effectiveness. Spain’s National Plan against Antibiotic Resistance (PRAN) 2025–2027 sets out a multisector, strategic framework to strengthen surveillance, control, prevention, training, and research as part of a coordinated response to this challenge. At the same time, recent advances in research on new vaccines, treatments, and diagnostic tools, driven by artificial intelligence (AI) and other technologies, are opening up promising pathways. These range from AI-assisted systems that improve the early detection of bacterial resistance, to more precise clinical decision-making, and projects that speed up the discovery of more effective antibiotics. Acting now is crucial if we want to ensure that antibiotics remain effective tools for protecting public health in the future.
For further details, see:
Agencia Internacional para la Investigación en Cáncer, Organización Mundial de la Salud. Estimated numbers from 2022 to 2050; Chin, Kah Wei, et al. “An overview of antibiotic and antibiotic resistance.” Environmental Advances nº 11, 2023; García, Pilar, et al. Bacterial Resistance to Antibiotics. Madrid: CSIC. Science for Public Policy, 2023; Ministerio de Sanidad, Ministerio de Agricultura Pesca y Alimentación y Ministerio para la Transformación Ecológica y el Reto Demográfico. “Plan Nacional Frente a la Resistencia a los Antibióticos 2025-2027.” Madrid, 2025; Mohsen, Naghavi, et al. “Global burden of bacterial antimicrobial resistance 1990–2021: a systematic analysis with forecasts to 2050.” The Lancet Public Health 0, 2024; Pennisi, Flavia, et al. “Artificial intelligence in antimicrobial stewardship: a systematic review and meta-analysis of predictive performance and diagnostic accuracy.” European Journal of Clinical Microbiology & Infectious Diseases 44. 2025; Peñalva, Germán, et al. “Burden of bacterial antimicrobial resistance among hospitalised patients in Spain: findings from three nationwide prospective studies.” The Lancet Regional Health Europe 51, 2025; and, Ritchie, Hannah y Edouard Mathieu. “How many people die and how many are born each year?”
The data shown in the chart are available at: OCDE. Pharmaceutical market [Pharmaceuticals consumption-Antibacterials for systemic use].